Summary
Cutaneous sepsis is a topical issue in international research, with high mortality and high incidence of organ dysfunction, which makes it necessary and beneficial early detection of sepsis, for the rapid initiation of appropriate systemic treatment, from the first hours after diagnosis. Any type of skin infection - bacterial, viral or fungal - can cause sepsis, but the most common are bacterial infections. Vasculitis, such as Gougerot-Ruiter trisyndrome, can cause sepsis, especially if the patient has other pathologies that contribute to the onset of a complex cascade, of disturbances of several organs and systems, with their functional insufficiency.
Gougerot-Ruiter trisyndrome or allergic leukocytoclastic vasculitis is characterized by damage to the arterioles and postcapillary venules, in the triggering of which several factors intervene (infections, drugs, autoimmune). Gougerot-Ruiter trisyndrome frequently presents as palpable purpura with elective localization in the lower half of the body, the evolution being acute, subacute, or chronic.
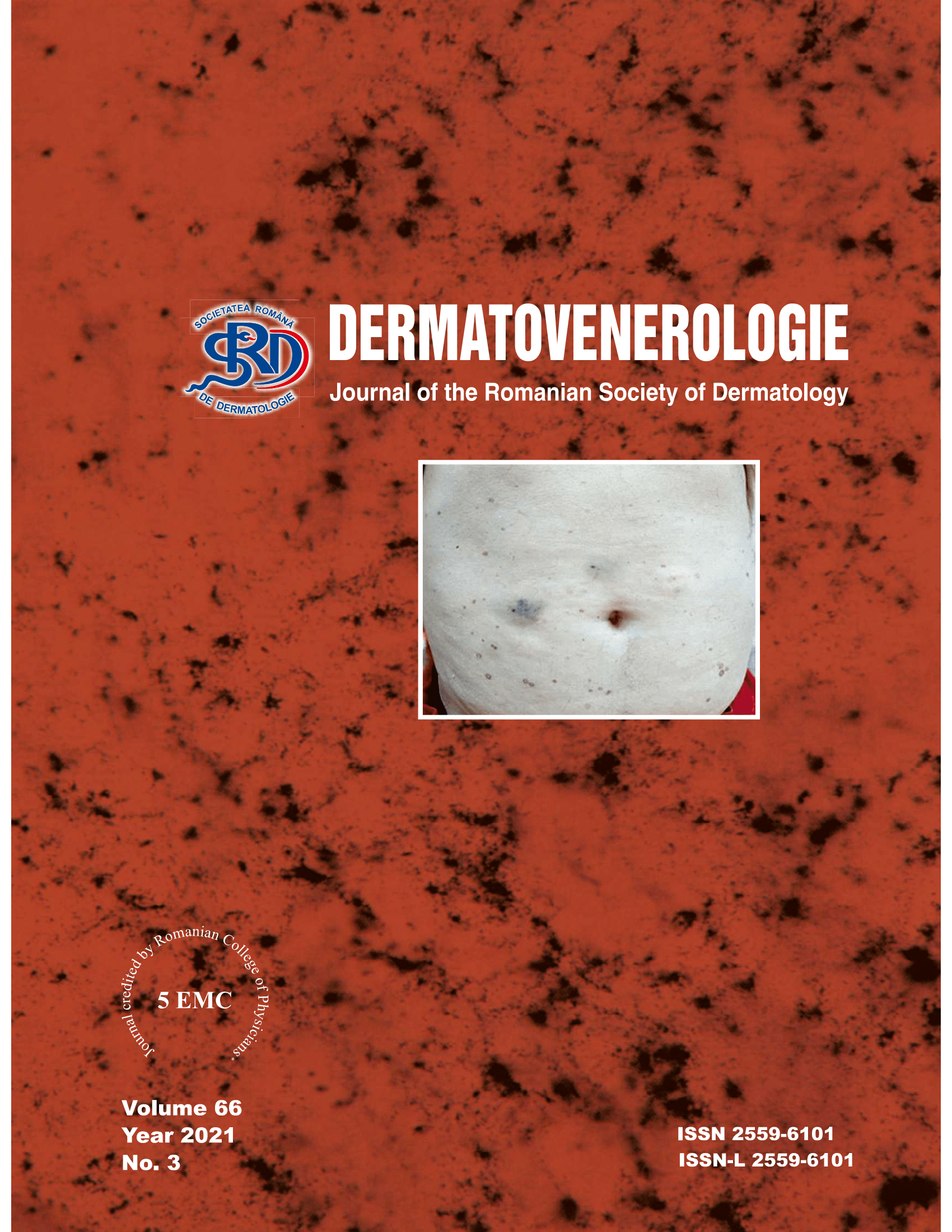
We present the case of a 60-year-old male patient with multiple cardiovascular, metabolic, gastroenterological comorbidities and numerous associated risk factors (smoker, overweight), who presented to the dermatology clinic for macular-papular-purpuric lesions and micronodules with a necrotic center, some isolated (abdomen, thighs), others confluent at the level of the calves in the form of painful and itchy necrotic ulcerations, with the onset of about 3 weeks, initially localized at calves and later with their extension after the thighs and abdomen. The patient did not follow topical or systemic treatment at home. Starting from the clinical and paraclinical elements, taking into account comorbidities and risk factors, the diagnosis of cutaneous sepsis was established, with vasculitis being the trigger. Elevated values of inflammatory biomarkers led to early initiation of antibiotic therapy, anticoagulant treatment, and corticosteroid therapy, which was performed in short courses and was limited by unbalanced glycemic status. The evolution was favorable, but slow, due to the inflammatory constellation of pre-existing pathologies.
The prognosis of patients with Gougerot-Ruiter trisyndrome is usually favorable, the skin damage being frequent, but the possibility of complications when there are associated pathologies must be evaluated.