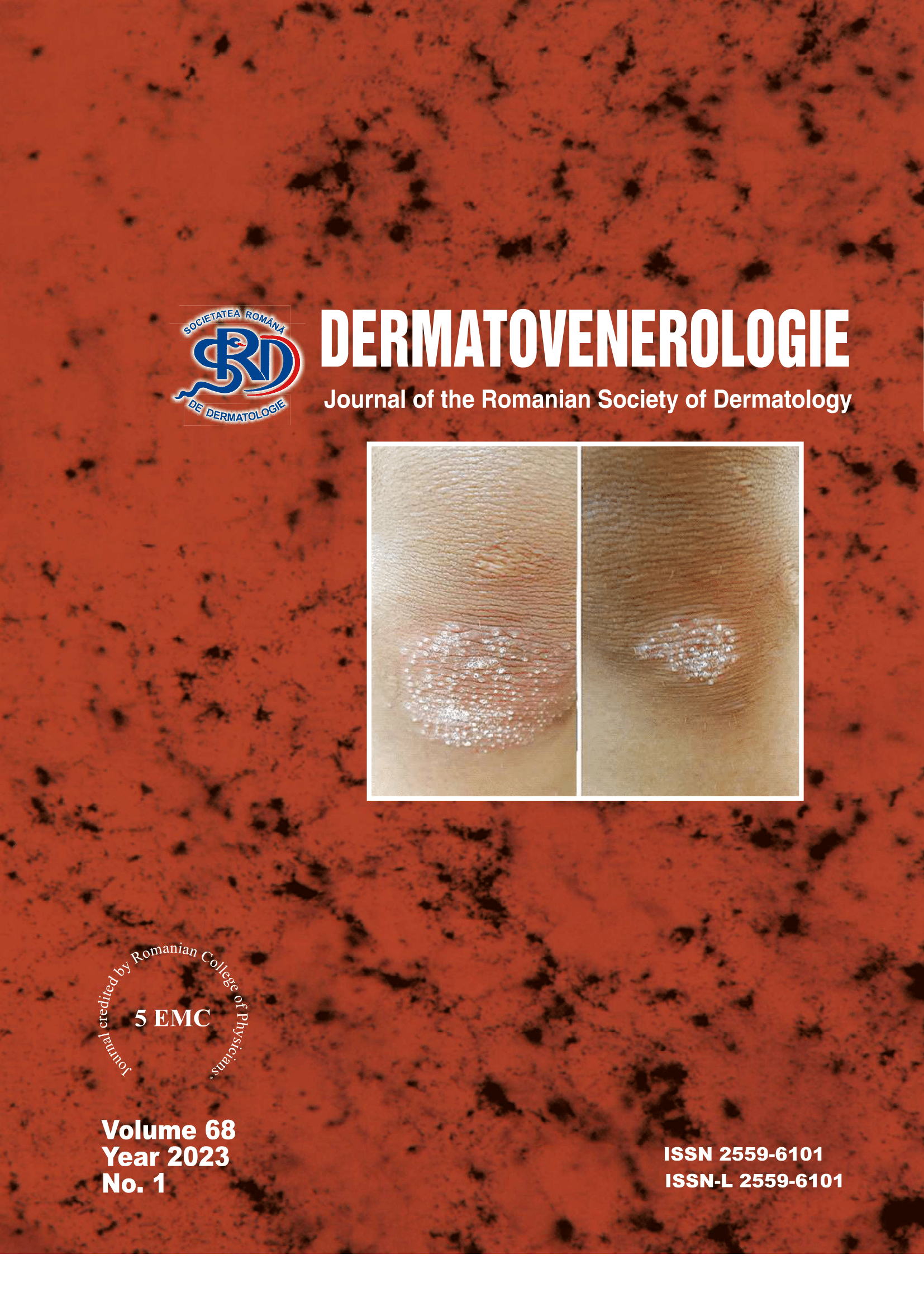
Rezumat
Psoriazisul este o boală cronică, inflamatorie, multisistemică a cărei debut este declanşat de factori genetici şi de mediu. Psoriazisul a fost asociat cu o gamă largă de comorbidităţi: sindrom metabolic, artrită psoriazică, boli cardiovasculare, tulburări psihice, neoplazii, precum şi boli inflamatorii intestinale. La momentul actual, pacienţii afectaţi de psoriazis pot beneficia de noi opţiuni terapeutice sigure şi eficiente. Cu toate acestea, pentru pacienţii afectaţi atât de psoriazis, cât şi de boli inflamatorii intestinale, se recomandă evitarea terapiei biologice cu inhibitori de interleukină 17, deoarece aceştia pot declanşa o exacerbare a simptomelor gastrointestinale. Mai mult decât atât, în literatura de specialitate a fost raportată prezenţa bolii inflamatorii intestinale la pacienţii cu psoriazis sub terapie biologică cu inhibitori de interleukină 17. În această lucrare prezentăm cazul unui pacient de sex masculin în vârstă de 33 de ani cu istoric îndelungat de psoriazis sub tratament cu inhibitori de interleukină 17, tratat anterior cu metotrexat. Pe durata terapiei imunosupresoare cu metotrexat, pacientul a menţionat prezenţa unor simptome gastrointestinale uşoare, care au persistat şi după iniţierea terapiei biologice. La acel moment, pacientul a corelat aceste simptome cu obiceiurile alimentare necorespunzătoare. Cu toate acestea, pacientul a fost îndrumat către secţia de gastroenterologie pentru investigaţii suplimentare. Corelaţia dintre nivelurile calprotectinei fecale, rezultatul colonoscopiei şi interpretarea histopatologică a biopsiilor din ileonul terminal a permis diagnosticarea unei ileite de tip Crohn posibil apărută în contextul terapiei biologice cu un inhibitor de interleukină 17. Abordarea terapeutică a constat în încetarea terapiei biologice cu secukinumab şi administrarea de corticoterapie sistemică, obţinându-se un control adecvat al bolii inflamatorii intestinale. Managementul psoriazisului a constat în iniţierea terapiei biologice cu risankizumab, un inhibitor de interleukină 23.