Summary
Pemphigus vulgaris (PV) and pemphigus foliaceus (PF) are bullous dermatoses with multiple similarities. The transition between these pemphigus subtypes rarely occurs and the underlying pathophysiological and molecular mechanism has been widely debated in many studies. The desmogleins are abundant in the hair follicles, which are frequently affected by acantholysis. The humid environment which is specific to the lesions promotes bacterial colonization.
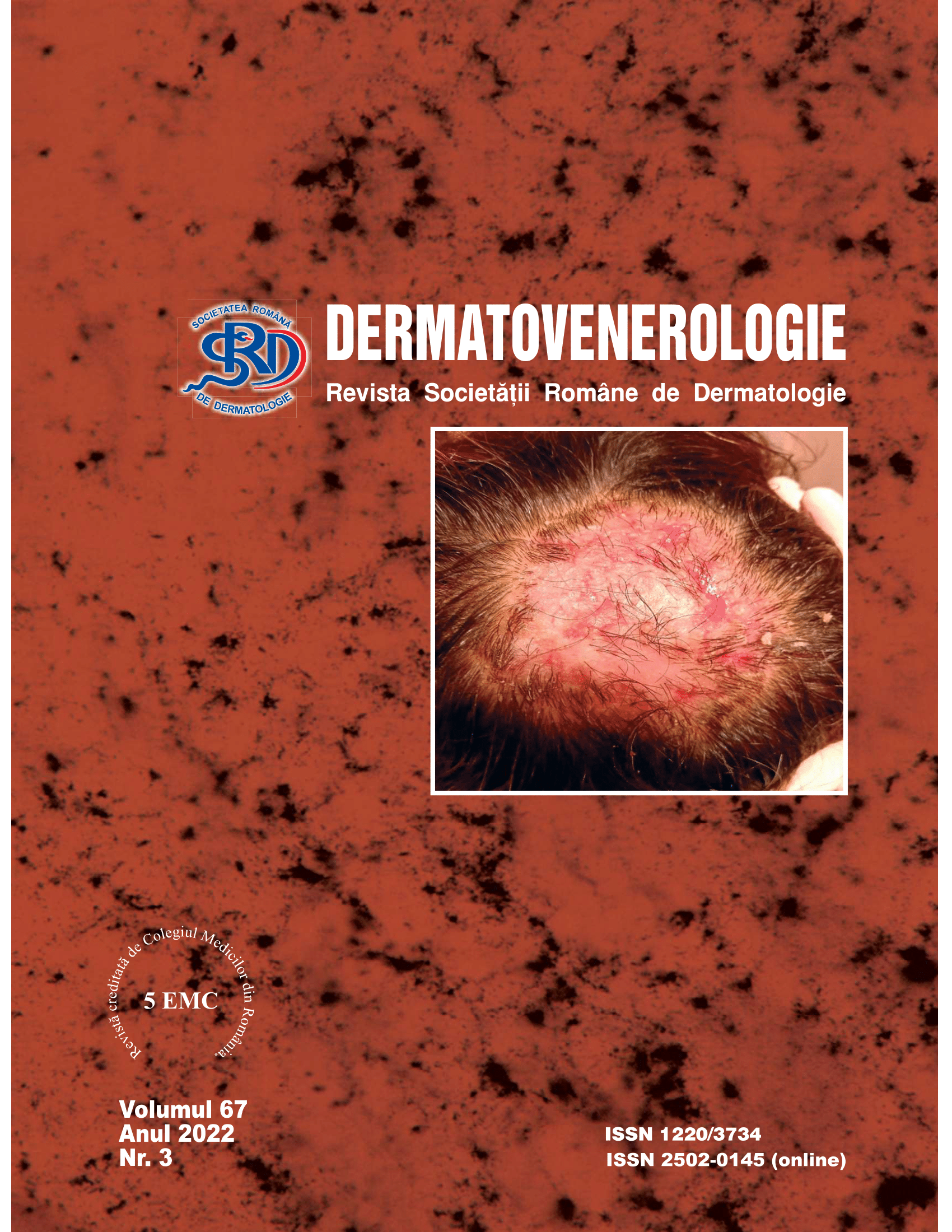
We present the case of a 49-year old patient diagnosed with PV in 2006, treated chronically with prednisone, who attended a consultation due to the appearance of an erosive lesion on the vertex of the scalp. The medical history shows the presence of a recurrence with an unchanged characteristic, which was triggered by the disruption of the treatment. The microbiologic culture of the secretion has confirmed the presence of Staphylococcus aureus each time the patient had a consultation. The anti-desmoglein 1 antibodies (anti-Dsg1) were found positive, and the histopathology exam revealed acantholysis at the subcorneal level, and in the granular layer. The flare was treated by increasing the dosage of the prednisone.
Although the scalp involvement is common in PV, the recurrent unilateral injury together with the appearance of nonscarring alopecia, while concomitant with a suprainfection, is specific to our case.We suspect the transition from PV to PF with an unchanged, recurrent nature, and discuss the role of suprainfection in the development of nonscarring alopecia.