Summary
Generalized pustular psoriasis (GPP) has traditionally been considered a variant of psoriasis vulgaris, especially since the two conditions often occur in the same patient.
However, recent research has proven that different pathological mechanisms are involved in the two conditions. The IL-36 in excessively activates in GPP and lead to an aberrant inflammatory response. Thus, GPP should be reclassified as a separate entity.
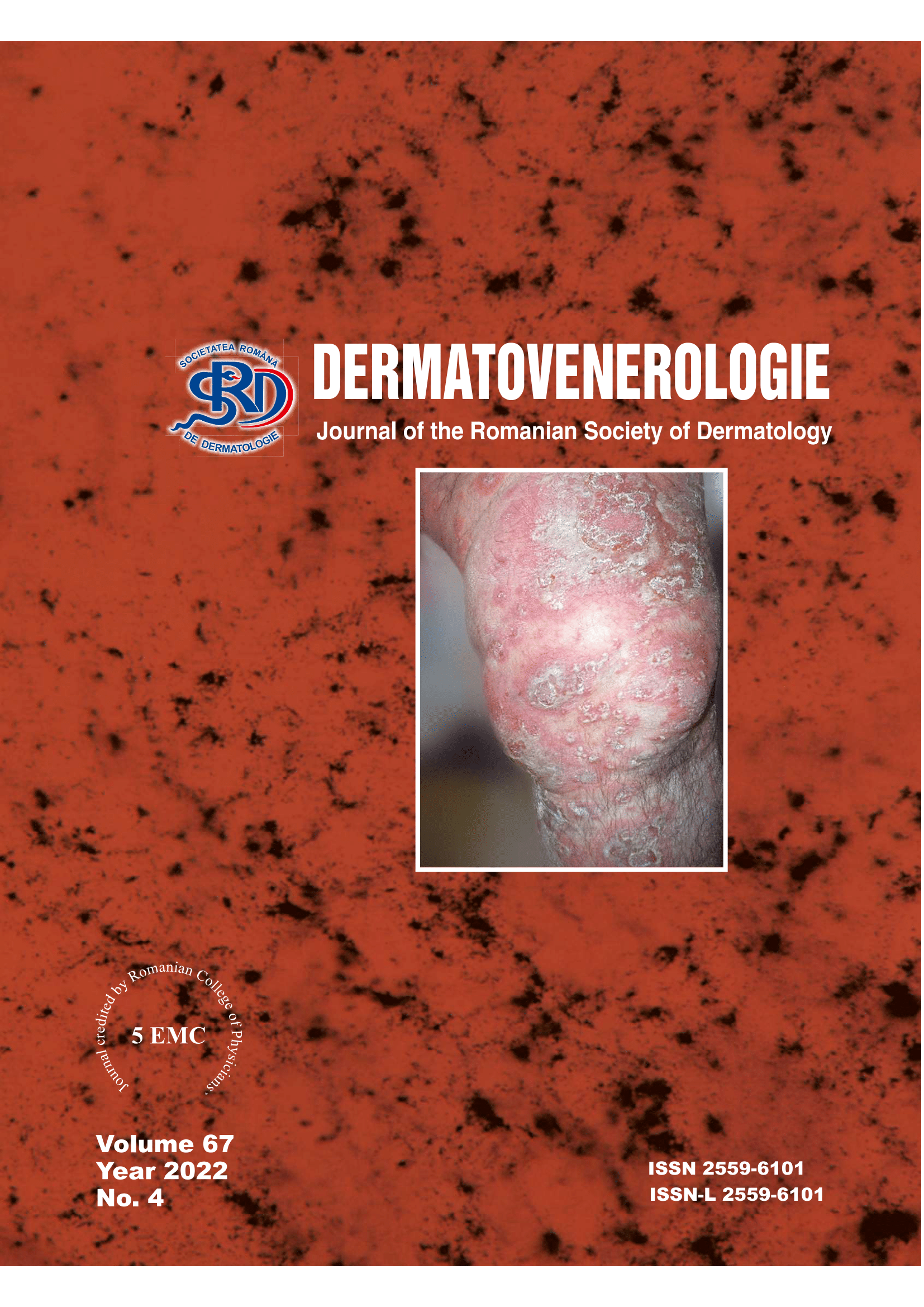
We present the case of a 51 year old patient, with a personal history of psoriasis vulgaris, who was admitted to our hospital for a generalized erythematous eruption, with overlying scales and pustules, occurring after emotional distress and excessive sun exposure. The patient’s history, clinical and histopathological examination were consistent with the diagnosis of GPP. Corticosteroids and methotrexate treatment was prescribed and the cutaneous eruption significantly improved during hospitalisation.
At the moment, the first line treatments for GPP are acitretin, methotrexate, cyclosporine and biological therapies. A better understating of the underlying physiopathological mechanisms involved in this disease and the development of new drugs that specifically target the involved pathways could lead to a more effective disease management in the future.
Clinical cases
GENERALIZED PUSTULAR PSORIASIS – A CASE REPORT AND THERAPEUTIC PERSPECTIVES